Author: Maame Ekua I believe there is a point where art and science meet and through visual communication we can contribute to…
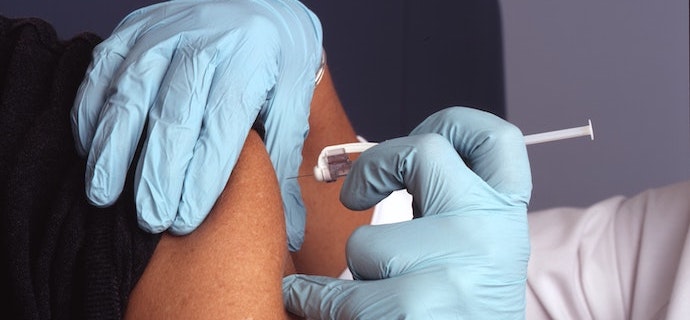
Who Gets the Vaccine? To ensure vulnerable populations get priority access to a COVID-19 vaccine, we need better health data
Authors: Debra Winberg, Janani Jayesh, Thomas Roades, Dr. Andrea Feigl and Dr. Jenna Patterson of the Health Finance Institute
As unfurling the complexities of COVID-19 continues to pose difficulty for global health specialists, emerging data from the pandemic is a constant reminder of the interconnectedness of non-communicable disease (NCDs) with this new virus. Populations with underlying chronic conditions are far more likely to be susceptible to the health risks posed by COVID-19, and at their intersection lies the dire need to find a solution to reduce population vulnerability and loss of lives.
It comes as no surprise that low-income countries have been hit the hardest by the joint COVID and NCD pandemic. As the world struggles to find ways to provide essential services to NCDs patients, disruptions to care have risen in response to the number of COVID-19 cases in a country. Due to the postponement of screenings and treatment as well as staff shortages, many patients with chronic conditions such as hypertension, diabetes, and cancer have had to reevaluate their treatment plans or forego treatment altogether. The brightest beacon of hope to ensure treatment continuity for such patients lies in the development of a COVID-19 vaccine, but the distribution of such a vaccine raises its own challenges.
Development of a COVID-19 vaccine
Since the start of the COVID-19 pandemic, the world has been racing to create a safe and effective vaccine. According to the WHO, as of August 13th there were 29 candidate vaccines in clinical evaluation and 138 candidate vaccines in preclinical trials. The development of a safe and effective COVID-19 vaccine would offer an opportunity for people to begin to return to the ‘new normal’ life.
Estimates of when a vaccine will be launched vary from the end of 2020 to the middle of 2021. There is, however, consensus that when the vaccine is launched, doses will be in short supply and governments and/or public health agencies will have to decide who gets the vaccine first.
Vaccines are a public good, meaning society as a whole benefits from them being administered to an individual. Yet some people benefit more than others by getting a vaccine — those at high risk of infection (i.e. healthcare and frontline workers) and those more likely to experience severe infection or mortality (i.e. the elderly and patients with chronic conditions). A WHO report in early September suggested using a tiered system for distribution for vaccine distribution and suggested that those aforementioned high-risk groups be included in Tier 1. But on a tiered roll-out basis, how do we ensure decisions on who gets vaccinated first are evidence-based?
The importance of data collection
More than likely, the number of people in at-risk groups will outnumber the first batch of available vaccines, which will result in stricter resource allocation. The WHO hopes that initial production from COVAX, the global vaccine cooperative, will be sufficient to cover about 20% of most countries’ populations. Ideally, that 20% should include frontline workers, the elderly, and those with underlying conditions. Understanding which groups to vaccinate first for the greatest degree of public good, however, requires more data than we currently have. Collecting data on NCDs, COVID-19, and the relationship between the two is vital to allow decision-makers to understand which groups should be vaccinated for maximum reduction in infection rates, hospital admissions, healthcare spending, and mortality.
NCD data can be hard to access; it’s often outdated and is rarely localized. Without access to current, high quality, granular data, policymakers and epidemiologists cannot accurately identify who should be among the first to receive a COVID-19 vaccine.
Forecasting is used for prioritization
With proper data, decision-makers can use epidemiological-economic forecasting models to help inform their allocation decisions. A form of operational research, forecasting allows decision-makers to compare the impacts of different alternatives before decisions are made — providing a mini experimentation without the risks of health and economic losses. These forecasting models synthesize clinical, epidemiological and economic evidence from various sources and help us understand which decisions would lead to the largest number of positive health outcomes and lowest economic costs. These models, however, are only as valid as their data inputs and without proper data, projections may lead us in the wrong direction.
So, where does that leave us?
Developing an effective and valid framework to distribute vaccines is essential for countries to transition seamlessly to the next phase of pandemic response. However, as time goes on the confusion seems to be mounting, and the lack of data is making public health experts scratch their heads. Although we know NCD patients are at a much higher risk of contracting COVID and suffering from more severe symptoms, we need solid datasets and evidence to point us to proper allocation of vaccines. This is especially crucial if we want to protect exceedingly vulnerable populations.