Silent killers: the scourge of noncommunicable diseases in Africa by Kofi Gunu
By Kofi Gunu
When global health leaders gather in Geneva this month to elect a new head of the World Health Organization, President Trump’s shadow will hang over the conclave. His “America First” agenda is a repudiation of the global consensus that has made the WHO effective at improving quality of life around the globe. Thus, the new director-general can expect to confront an ever growing list of threats with a smaller toolset. That would portend poorly for the fight against the most urgent health crisis facing Africa today: the rise of noncommunicable diseases (NCDs).
The NCD epidemic in Africa is of an intensely personal interest to me. Growing up in Ghana, I contracted not only the usual childhood illnesses but managed to survive frequent bouts of cholera and malaria. Joining a U.S.-based non-profit operating primary health facilities in my home country as a young adult, I anticipated dealing exclusively with the tropical infections that plagued my childhood. To my surprise, nearly half of our patients were diagnosed with ailments one is more likely to find in a doctor’s office in suburban America: diabetes, cancer, cardiovascular disease, and chronic respiratory illness. These NCDs, not the “third world” maladies more commonly associated with Africa, now threaten to derail progress on the continent.
Africa has undoubtedly made great strides in health-care delivery within the last decade. In collaboration with development partners, many African countries have significantly improved the life expectancy of their people. Childbirth and tuberculosis (TB) are no longer the death sentences they used to be. Today, 11.5 million people in sub-Saharan Africa have access to antiretroviral therapy, up from 50,000 in 2003. Expected to double in population within the next generation, Africa today stands on the cusp of a “demographic dividend,” with young working-age people projected to vastly outnumber both young and old dependents, combined.
These gains will all be erased, however, if the current rise in NCDs is permitted to continue unabated. NCDs are projected to be the leading cause of death in sub-Saharan Africa by 2030. In most North African countries, they are already responsible for more than three-quarters of all nonviolent deaths. And young people like me are the primary victims. In sub-Saharan Africa, people who succumb to cardiovascular disease die on average 10 years earlier than in developed countries. Unless immediate action is taken, the emerging NCD epidemic will put tremendous pressure on already overburdened health-care systems and pose serious challenges to sustainable development in Africa.
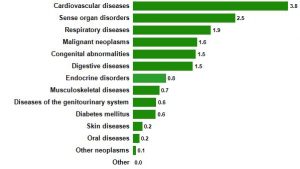
Most experts attribute the decline in Africa’s infectious disease burden to sustained global leadership and investment. In 2002, donor countries, nongovernmental organizations, and philanthropic institutions came together to launch the Global Fund to Fight AIDS, tuberculosis, and malaria; and in 2003, the U.S. government established the President’s Emergency Plan for AIDS Relief (PEPFAR). Together, these programs have immunized and treated millions of Africans each year, and channeled billions of dollars toward the research and development of new and highly effective interventions.
A comparable outpouring of international support is needed to address the major factors driving the NCD crisis. Such an effort, to be truly consequential, should move beyond targeting particular diseases to creating world-class health systems on the continent. Moreover, emerging markets, especially China and India, need to be enlisted in promoting better health outcomes in Africa. Increased international engagement on the rising NCD epidemic is imperative to achieving a peaceful and more prosperous world.
VICTIMS OF SUCCESS?
Paradoxically, the current rise in the number of people contracting NCDs in Africa can be traced to higher life expectancies worldwide. According to data published by the World Bank, life expectancies increased, on average, by six months per year in low-income countries, particularly on the African continent, between 2000 and 2012. Many of the NCDs on the rise are associated with aging, and it follows that as lifespans grow, more people are coming down with these conditions. But, as the Task Force Report released by the Council on Foreign Relations (CFR) points out, this explanation fails to adequately account for the prevalence of NCDs among a much younger segment of the population, with much worse health outcomes, in developing countries compared to wealthier counterparts.
It should come as no surprise that marked health disparities persist between rich and poor countries, despite the successes of the last decade. Health spending by African governments has struggled to keep pace with changing health priorities. As the CFR report well notes, the combined health budget of all governments in sub-Saharan Africa is just a little more than what the Polish government spends on health annually. As a result, the health-care systems in these countries remain ill-equipped to provide the preventive and chronic care that at-risk populations need.
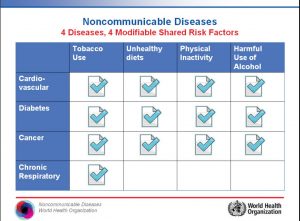
These systemic problems are further exacerbated as African populations become more urbanized and better integrated into the global market. Rapid improvements in the ease with which goods and people travel across the globe have increased Africans’ exposure to tobacco products, alcohol, and processed food and beverages, fueling poor health habits. It is impossible to overstate the positive role globalization has played in Africa’s development in recent years, from lifting millions out of abject poverty, increasing crop yields, and eradicating diseases, such as guinea worm, in all but a few countries. At the same time, it is the case that globalization shares part of the blame for the NCD epidemic sweeping the continent. Unlike high-income countries who also grapple with the health impact of modernization, African countries lack the basic consumer protections and public health infrastructure necessary to prevent NCDs.
THE TOLL OF NONCOMMUNICABLE DISEASES
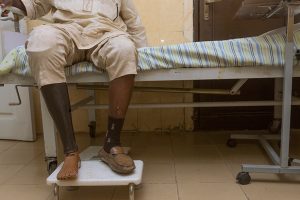
The NCD problem is wreaking economic and social havoc in many African countries. Governments now have to devote scarce health-care resources to taking care of patients who, due to the chronic nature of NCDs, are sick longer and require specialized medical attention. This often means depleting funds reserved for combating infectious and nutritional diseases that remain health threats in several countries. Premature deaths and disability from NCDs represent a major drain on national labor supplies and diminish workforce productivity. A World Bank study, for example, discovered that NCDs reduce the labor supply in Egypt by approximately 19 percent, a GDP loss of 12 percent. For all its promise, Africa’s demographic dividend might yet fail to yield the same benefits it brought to high-income countries, thanks to NCDs.
Meanwhile, NCDs have brought untold hardship to ordinary individuals and households. I witnessed this devastation first-hand during my internship in Ghana. The exorbitant out-of-pocket costs associated with NCD treatments forced many poor families I knew into making painful financial choices. In rural Ghana, minimum-wage earners with diabetes spend up to 60 percent of their incomes on insulin. Sadly, those are the lucky ones. Premature death and disability from NCDs deprive countless families of their primary breadwinners.
The human and economic toll of NCDs is undermining the painstaking gains made in recent years by public health programs targeted at communicable diseases. NCDs cause premature death and disability in the very same populations that PEPFAR and the Global Fund are saving from AIDS, malaria, and other diseases. According to recent research, PEPFAR patients in Africa disproportionately suffer from rising rates of NCDs including renal disease, chronic respiratory illnesses, and cervical cancer. In a costly way, the NCD epidemic has exposed the folly of obsessing on certain ailments to the neglect of others. Spending billions of dollars to save individuals from one preventable and treatable disease only for them to succumb prematurely to another preventable and treatable disease is an outcome as tragic as it is wasteful.
A NEW GLOBAL COMMITMENT
We can do better. Farsighted African leaders must lead the way in convening major global health actors—donor countries, nongovernmental organizations, and philanthropic institutions—to develop a practical, sustainable, and well-prioritized plan for collective action. To have a real impact, such a plan should prioritize two goals above all else. First, it should propose ways to update the health systems in African countries to meet the demand for both primary and long-term care. The NCD problem arose, even as programs like PEPFAR were touted as successes, because those earlier initiatives focused narrowly on AIDS or malaria or TB and ignored a host of health risks lurking just outside the limelight of international attention. A far more effective way to help Africa on NCDs is to improve the continent’s overall health-care environment.
This upgrading will require increased financing, more and better trained medical professionals, and state-of-the-art facilities for research and treatment. It will demand that governments strengthen consumer protection laws designed to encourage responsible health habits but which are notoriously lax due mainly to the machinations of multinational corporations. Of course, part of such an effort will be creating NCD programs across the continent, but these should be done in the context of raising African health systems to world-class standards.
Second, the plan should create the platform for African countries to collaborate with one another and with other developing countries in devising effective prevention mechanisms. African governments should prioritize NCD management in development partnerships with emerging markets, especially China and India. As, perhaps, Africa’s most significant trade and diplomatic partners in the 21st century, China and India are indispensable to a resilient future for the continent. Both countries are grappling with enormous NCD burdens of their own, and African countries have much to learn from their successes and failures in this regard.
The NCD crisis is the defining challenge facing African countries today. It threatens to obliterate the public health progress that has been achieved on the continent in the last decade. Young Africans like me are looking up to our leaders and to the world to save our generation and reclaim the promise of a resurgent Africa.
References
- “Antiretroviral Therapy (ART) Coverage among All Age Groups.” World Health Organization. World Health Organization, n.d. Web. 15 Oct. 2016.
- Marquez, P. V., Farrington, J. L. (2013) “The Challenge of Non-Communicable Diseases and Road Traffic Injuries in Sub-Saharan Africa. An Overview”. Washington, DC.: The World Bank.
- “Noncommunicable Diseases Country Profiles 2014.” World Health Organization. World Health Organization, n.d. Web. 15 Oct. 2016.
- World Development Indicator Tables, “Life Expectancy at Birth (Total Years),” World Bank, http://data.worldbank.org/indicator/SP.DYN.LE00.IN.
- Independent Task Force Report No. 72. “The Emerging Global Health Crisis.” Council on Foreign Relations. Council on Foreign Relations, Dec. 2014.
- OECD (Organization for Economic Cooperation and Development) Health Stats, “Public Health Expenditure Since 2000,” via Organization for the Economic Cooperation and Development, http://stats.oecd.org/index.aspx?DataSetCode=HEALTH_STAT.
- Lorenzo Rocco et al., “Chronic Diseases and Labor Market Outcomes in Egypt,” World Bank Policy Research Working Paper 5575 (2011), doi: 10.1596/1813-9450-5575.
- Ama de-Graft Aikens, “Healer Shopping in Africa: New Evidence From Rural-Urban Qualitative Study of Ghanaian Diabetes Experiences,” BMJ vol. 331 (2005), doi:http://dx.doi.org/10.1136/bmj.331.7519.737.
- Lisa R. Hirschhorn et al., “Cancer and the ‘Other’ Noncommunicable Chronic Diseases in Older People Living With HIV/AIDS in Resource-Limited Settings: A Challenge to Success,” AIDS vol. 26 (2012), pp. S65-S75.

Kofi Gunu will graduate this May from Augustana University in Sioux Falls, South Dakota, with majors in political science and economics. Kofi has participated in multiple internships, including helping Sanford Health build new clinics in his home country of Ghana. He conducted research with the Council on Foreign Relations’ Thomas Bollyky into the growing global health burden in developing countries. Starting in August 2017, he will be spending a year in China as a Schwarzman Scholar. ckgunu13@ole.augie.edu
__________________________________________________________________
Opinions expressed in this post reflect solely the views of its author and are not necessarily shared by PLOS or the PLOS journals.

[…] Source: Silent killers, the scourge of noncommunicable diseases in Africa by Kofi Ganu […]
The essence of Kofi Gunu’s message is that the goal of all health services, national and international is health for all. Achieving this goal would be the best way of preventing and reducing all communicable and non-communicable diseases, and in my opinion can be accomplished by focusing on. the pursuit of health by all and for all. This is because the pursuit of health is both a personal and collective responsibility. Furthermore since it is less difficult and less costly to establish healthy behavior than to change change unhealthy behavior the pursuit of health should be a life long process.
Mr. Kofi has mentioned the torment of Non-Communicable Disease Africa. We all know the aim behind all these
medical services is to cure diseases and provide better health to everyone. While chasing the goals of better health unheathly behaviour might be seen at some places, which is a prima facie.If the behaviour and the way of communication won’t be improved, there’ll be unforeseen events, which even after the cure of disease will continue to be a hot talk.